What does a final diagnosis of STEMI vs. NSTEMI depend upon?
Dr. Smith's ECG Blog
NOVEMBER 10, 2024
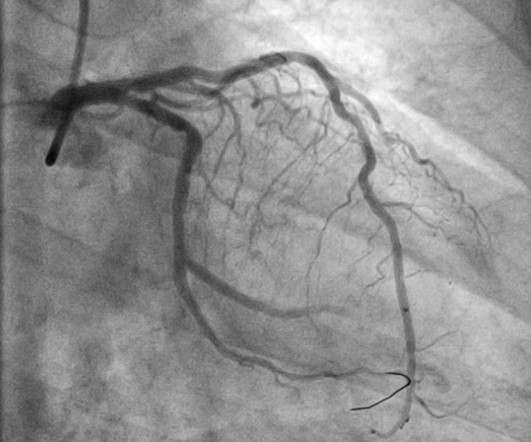
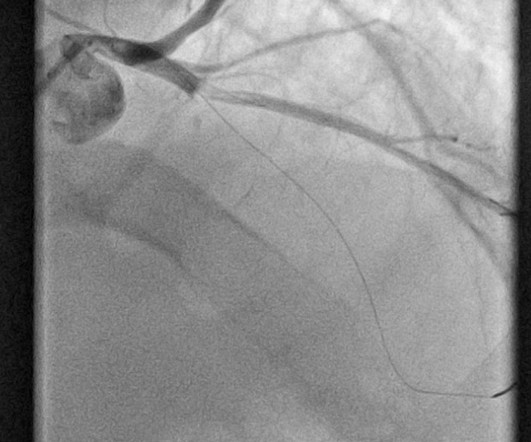
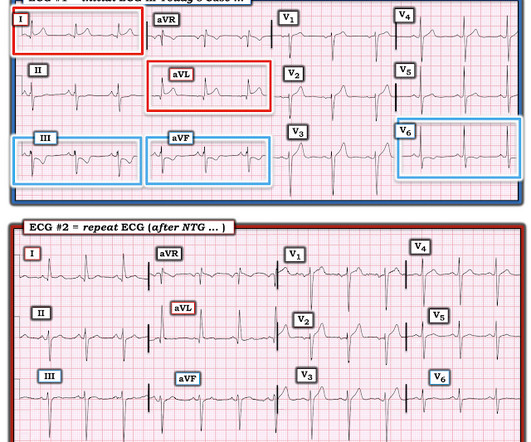
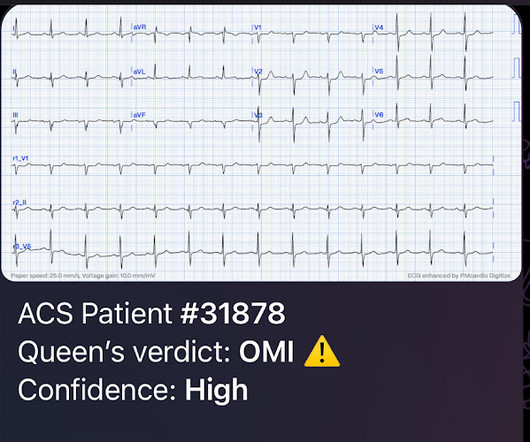
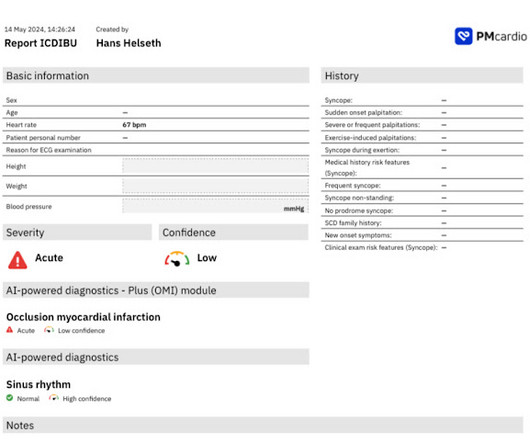
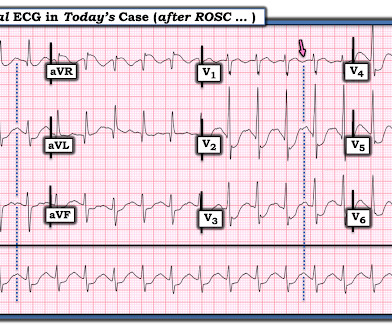
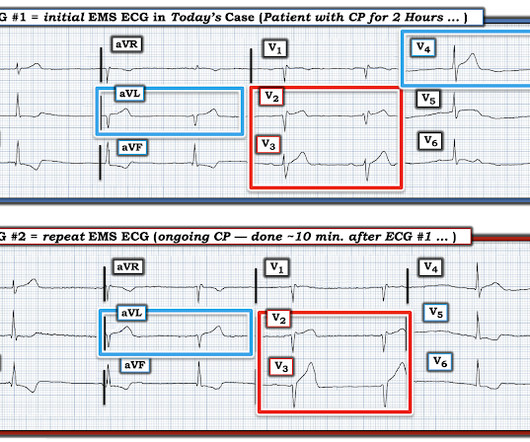
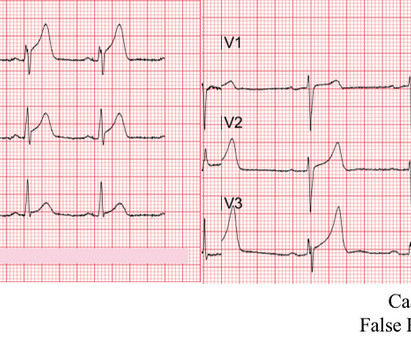
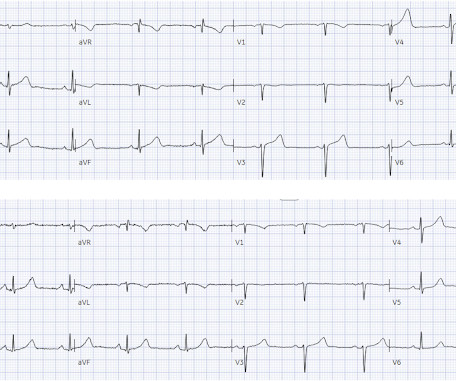
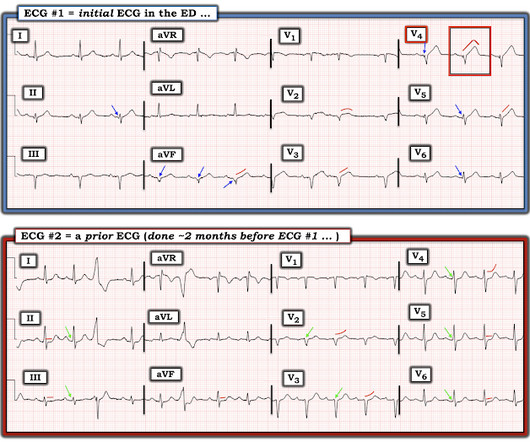
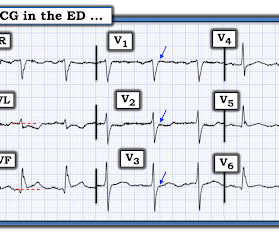
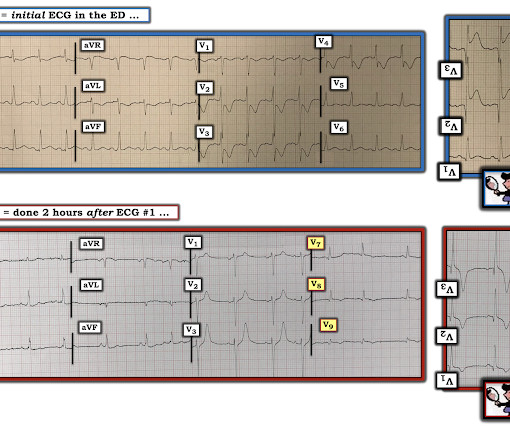
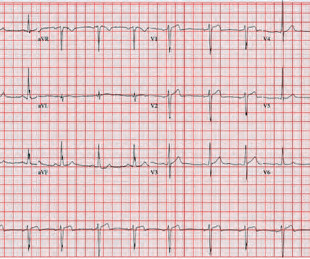
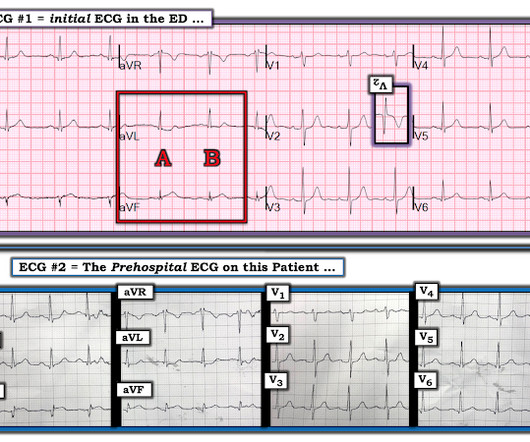
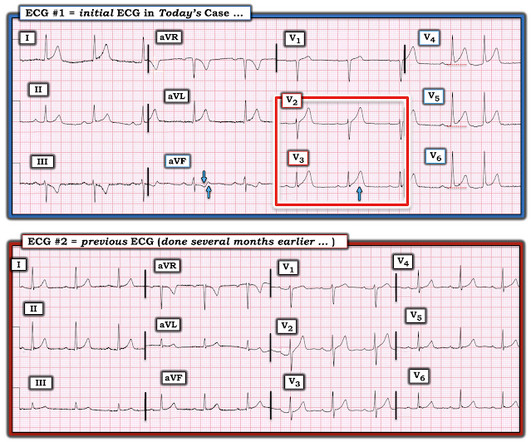
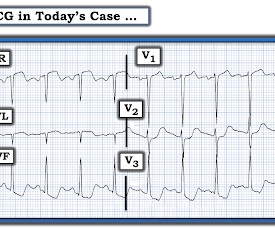
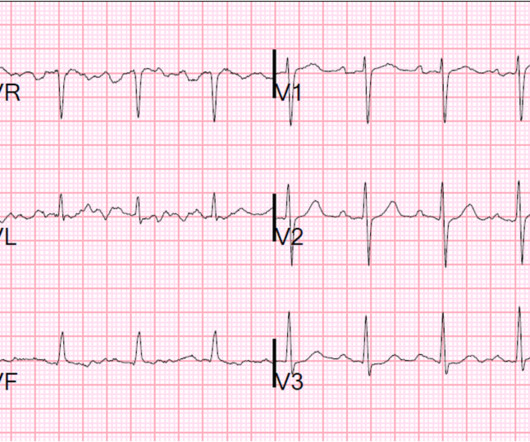
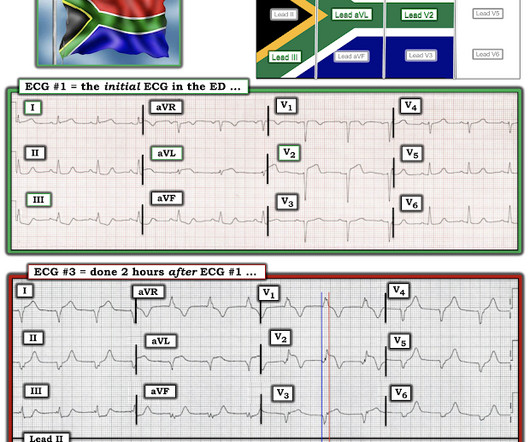
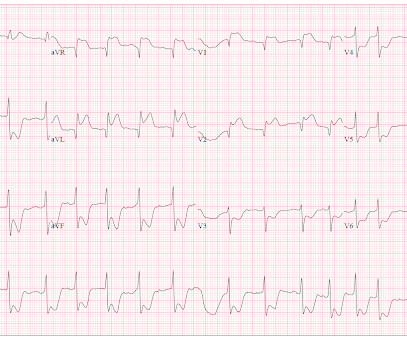
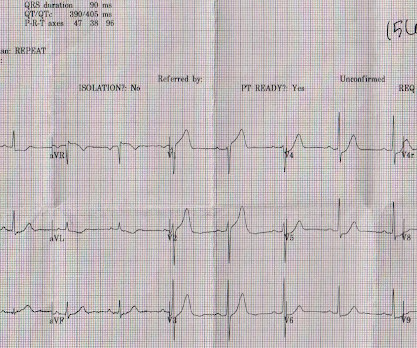
The is very small STE in III and aVF which do not meet STEMI criteria, hyperacute T waves, reciprocal TWI in aVL, and maximal STD in V2-V3 showing posterior OMI. The ECG was transmitted to the Emergency Medicine physician who recognized inferior and posterior OMI findings, and confirmed that the patient has potential ACS symptoms.

























Let's personalize your content