ECG Cases 48 – ECG Interpretation in Cardiac Arrest
Emergency Medicine Cases
FEBRUARY 13, 2024
The post ECG Cases 48 – ECG Interpretation in Cardiac Arrest appeared first on Emergency Medicine Cases.
This site uses cookies to improve your experience. To help us insure we adhere to various privacy regulations, please select your country/region of residence. If you do not select a country, we will assume you are from the United States. Select your Cookie Settings or view our Privacy Policy and Terms of Use.
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.
Used for the proper function of the website
Used for monitoring website traffic and interactions
Cookies and similar technologies are used on this website for proper function of the website, for tracking performance analytics and for marketing purposes. We and some of our third-party providers may use cookie data for various purposes. Please review the cookie settings below and choose your preference.

Emergency Medicine Cases
FEBRUARY 13, 2024
The post ECG Cases 48 – ECG Interpretation in Cardiac Arrest appeared first on Emergency Medicine Cases.

Emergency Medicine Cases
JUNE 6, 2023
In this ECG Cases blog we look at 10 patients with shortness of breath, and discuss how the ECG can be used to help diagnose cardiac, respiratory and metabolic emergencies.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.

Dr. Smith's ECG Blog
NOVEMBER 27, 2024
Doing so literally enables those of us who embrace the OMI Paradigm the ability to recognize within seconds that a patient with new CP ( C hest P ain ) — and — one or more hyperacute T waves — needs prompt cath regardless of potential absence of STEMI criteria. Figure-1: ECG from the August 26, 2009 post in Dr. Smith's ECG Blog.

Emergency Medicine Cases
JANUARY 17, 2023
In this ECG Cases blog we look at 9 patients with possible transient STEMI and discuss pitfalls and pearls in ECG interpretation and management. The post ECG Cases 39 – Transient STEMI Pitfalls and Pearls appeared first on Emergency Medicine Cases.

Emergency Medicine Cases
OCTOBER 22, 2019
In this ECG Cases blog we present ECGs from 7 patients who presented with chest pain and mild anterior ST elevation. Can you identify which were early repolarization and which were anterior STEMI? The post ECG Cases 2: Early Repolarization or Anterior STEMI? appeared first on Emergency Medicine Cases.

Emergency Medicine Cases
MARCH 10, 2020
10 patients presented with the "STEMI-equivalent" ST elevation in aVR with diffuse ST depression. Jesse McLaren guides us through the differential diagnosis of ST elevation in aVR with diffuse ST depression in this ECG Cases blog. The post ECG cases 7: ST elevation in aVR, STEMI-equivalent? Which had acute coronary occlusion?
Emergency Medicine Cases
DECEMBER 16, 2019
In this ECG Cases blog we look at seven patients with potentially ischemic symptoms and subtle ECG changes in the lateral leads. The post ECG Cases 4: Lateral STEMI or Occlusion MI? Which had acute coronary occlusion? Introducing the concept of Occlusion MI - a paradigm shift in ECG diagnosis of MI.
Emergency Medicine Cases
SEPTEMBER 21, 2021
In this ECG Cases blog we look at 10 patients with potentially ischemic symptoms. Jesse McLaren explains 'Late STEMI' and how reperfusion strategies should not be based on time of symptom onset. The post ECG Cases 25: ‘Late STEMI’ – How acute is the coronary occlusion?

Emergency Medicine Cases
AUGUST 8, 2023
In this ECG Cases blog with Dr. Jesse McLaren we interpret 10 ECG cases and explore cardiac, metabolic and GI causes: We consider anginal equivalents, and look for ECG signs of Occlusion MI, including subacute occlusion from delayed presentations.

Emergency Medicine Cases
MAY 10, 2023
In this ECG Cases blog we look at 10 cases of patients with chest pain, including false positive STEMI, false negative STEMI, and other causes to help hone your ECG interpretation skills in time-sensitive cases where those very ECG skills might save a life.
Dr. Smith's ECG Blog
OCTOBER 30, 2023
A 60 yo with 2 previous inferior (RCA) STEMIs, stented, called 911 for one hour of chest pain. Here is his most recent previous ECG: This was recorded after intervention for inferior STEMI (with massive ST Elevation, see below), and shows inferior Q-waves with T-wave inversion typical of completed inferior OMI. ng/mL (quite large).

REBEL EM
SEPTEMBER 28, 2023
Background: Primary PCI is the recommended reperfusion strategy in patients with STEMI and should be initiated within 2 hours after first medical contact. In non-PCI-capable hospitals this goal is not always achievable due to delays in transfer. In these cases, thrombolysis is recommended to improve morbidity and mortality. Primary PCI: 95.7%

EMDocs
DECEMBER 11, 2023
Traditionally, emergency providers looked for signs of ST-segment elevation myocardial infarction (STEMI) to indicate the need for intervention. Emergency physicians have recognized for some time that there are many occlusions of the coronary arteries that do not present with classic STEMI criteria on the ECG.

Emergency Medicine Cases
MAY 10, 2023
In this ECG Cases blog we look at 10 cases of patients with chest pain, including false positive STEMI, false negative STEMI, and other causes to help hone your ECG interpretation skills in time-sensitive cases where those very ECG skills might save a life.
Emergency Medicine Cases
APRIL 2, 2024
In this ECG Cases blog, Jesse McLaren and Rajiv Thavanathan explore how ECG and POCUS complement each other for patients presenting to the emergency department with shortness of breath or chest pain. They explain complementary diagnostic insights into pericardial effusion and cardiac tamponade, occlusion MI and RV strain.
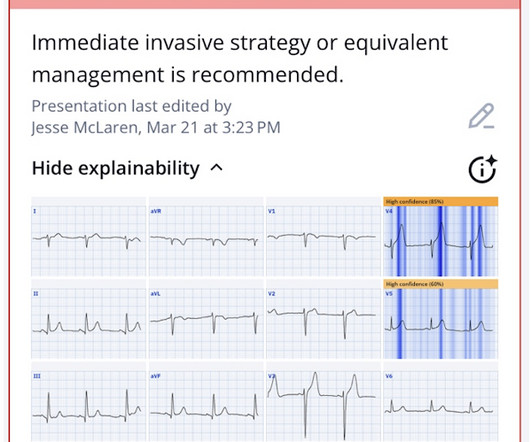
Dr. Smith's ECG Blog
MARCH 27, 2025
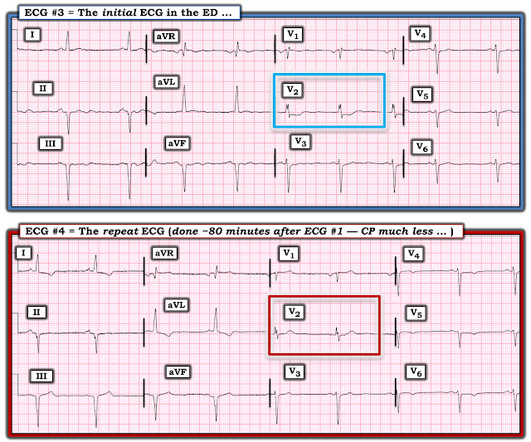
Theres ST elevation in V3-4 which meets STEMI criteria, which could be present in either early repolarization, pericarditis or injury. Lets see what happens in the current STEMI paradigm. Emergency physician: STEMI neg but with elevated troponin = Non-STEMI The first ECG was signed off. What do you think?

Dr. Smith's ECG Blog
DECEMBER 5, 2023
Beyond STEMI: Diagnosing Acute Coronary Occlusion on the ECG. The Queen of Hearts AI app can do it for you. With explainability too.

Emergency Medicine Cases
JUNE 21, 2022
In this ECG Cases blog we review 8 cases of patients with prehospital ECGs and explore prehospital ECGs for diagnosing STEMI, Occlusion MI, false STEMI, code STEMI, dynamic ischemic changes, truncated voltages. Can you avoid the pitfalls and spot the pearls that help to make the diagnosis?
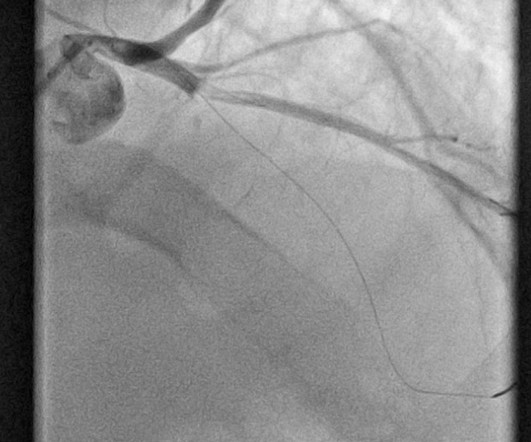
Dr. Smith's ECG Blog
SEPTEMBER 12, 2024
The paramedic called the EM physician ahead of arrival and discussed the case and ECGs, and both agreed upon activating "Code STEMI" (even though of course it is not STEMI by definition), so that the acute LAD occlusion could be treated as fast as possible. So the cath lab was activated. Long term outcome is unavailable.
Emergency Medicine Cases
DECEMBER 20, 2022
Jesse McLaren discusses some key aspects of cocaine chest pain ECG interpretation in this month's blog including: Patients with cocaine-associated chest pain require benzodiazepines +/- nitroglycerine for symptom relief, aspirin and ECG to look for signs of occlusion and reperfusion.

Emergency Medicine Cases
FEBRUARY 11, 2020
In this ECG Cases blog we look at 8 patients with potentially ischemic symptoms, none of whom had STEMI on the 12 lead ECG. Which had occlusion MI? The post ECG cases 6: Posterior MI – Still Under-recognized appeared first on Emergency Medicine Cases.
Emergency Medicine Cases
MAY 18, 2020
Seven patients with ischemic symptoms, none meeting STEMI criteria but all identified by a specific pattern of first diagonal branch occlusion are explored in this ECG Cases blog with Jesse MacLaren who also explains The South African Flag Sign.
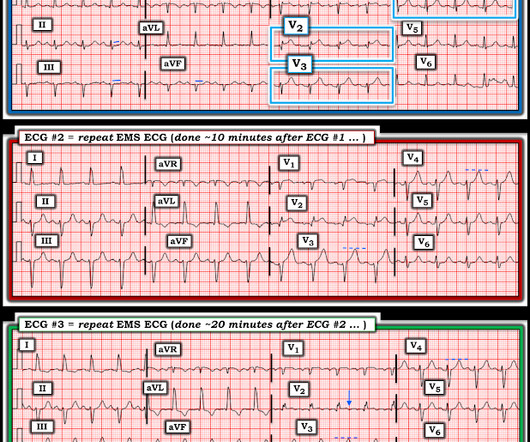
Dr. Smith's ECG Blog
JANUARY 3, 2024
Interpretation : diagnostic of acute anterior OMI with STE less than STEMI criteria in V1-V4, hyperacute T waves in V2-V4, and suspiciously flat isoelectric ST segments in III and aVF suspicious for reciprocal findings. Now it even meets STEMI criteria, and HATWs continue to inflate. So the cath lab was not activated. Ongoing OMI.
Emergency Medicine Cases
SEPTEMBER 15, 2020
LVH produces secondary repolarization abnormalities that can mimic STEMI. In this ECG Cases blog we look at 6 patients who presented with potentially ischemic symptoms and LVH on their ECG.
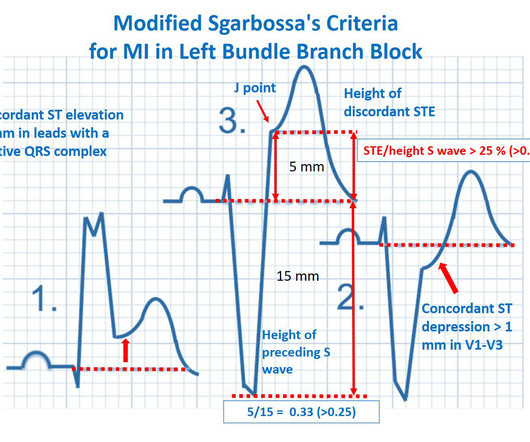
REBEL EM
JULY 5, 2023
If it looks and feels like a STEMI clinically, get serial ECGs and consult Cardiology immediately. Post Created By: William Caputo MD Post Peer Reviewed By: Anand Swaminathan MD, MPH (Twitter @EMSwami ) The post REBEL Core Cast 104.0 – Subtle ECGs in Acute Coronary Occlusion appeared first on REBEL EM - Emergency Medicine Blog.

Emergency Medicine Cases
OCTOBER 17, 2023
In this ECG Cases blog Dr. Jesse McLaren guides us through 10 cases, driving home the points that sepsis is a common cause of rapid Afib and diffuse ST depression with reciprocal ST elevation in aVR, myo/pericarditis is a diagnosis of exclusion, endocarditis or lyme carditis can cause AV block, PE can cause low grade fever and ECG signs of acute RV (..)
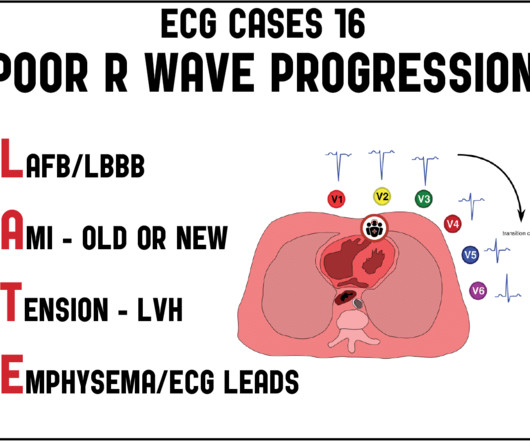
Emergency Medicine Cases
DECEMBER 8, 2020
In this ECG Cases blog we examine 6 patients who presented with poor R wave progression, and the LATE mnemonic for the differential. The post ECG Cases 16: Poor R-wave progression – The LATE mnemonic appeared first on Emergency Medicine Cases.
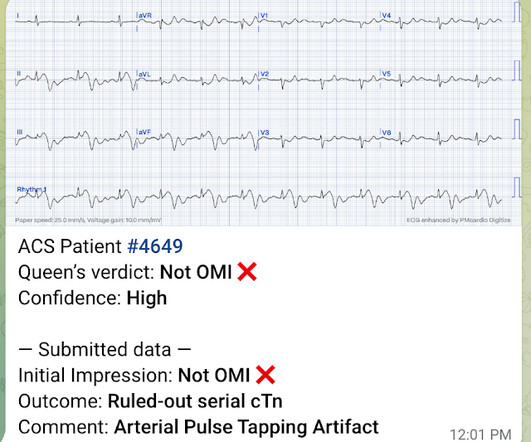
Dr. Smith's ECG Blog
SEPTEMBER 15, 2023
I came to work one day and one of my partners said, "Hey, Steve, we had a STEMI this afternoon!" That is not a STEMI. More cases can be found on the blog here. They had activated the cath lab and the interventionalist did not notice that it was not a STEMI/OMI. I said, "Cool, can I see the ECG?' He said: "What?
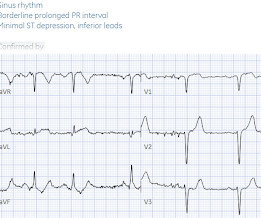
Dr. Smith's ECG Blog
JULY 7, 2024
So while there’s no diagnostic STEMI criteria, there are multiple ischemic abnormalities in 11/12 leads involving QRS, ST and T waves, which are diagnostic of a proximal LAD occlusion. First trop was 7,000ng/L (normal 25% of ‘Non-STEMI’ patients with delayed angiography have the exact same pathology of acute coronary occlusion.
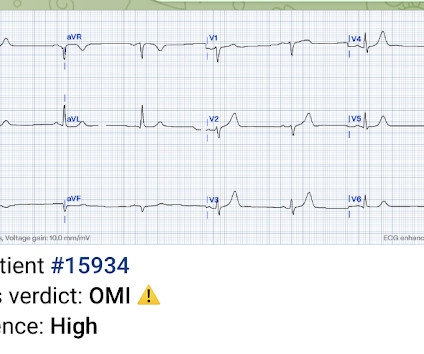
Dr. Smith's ECG Blog
MARCH 4, 2024
Unknown algorithm The Queen gets it right Case 4 How unreliable are computer algorithms in the Diagnosis of STEMI? The patient's prehospital ECG showed that there was massive STEMI and these are hyperacute T-waves "on the way down" as they normalize. Pain was resolving. Diagnosed as Normal by the computer. Troponin negative.
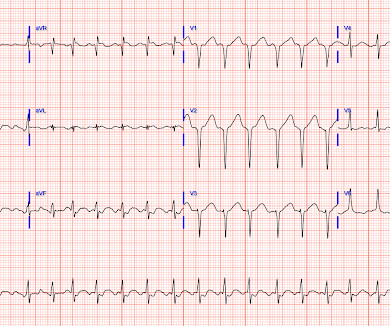
Dr. Smith's ECG Blog
JULY 9, 2024
Despite anticipation by many that the initial post-resuscitation ECG will show an obvious acute infarction — this expected "STEMI picture" is often not seen. Meyers and Smith in the October 15, 2022 post of Dr. Smith's ECG Blog ). Restoration of sinus rhythm is evident in Figure-1.

Dr. Smith's ECG Blog
APRIL 18, 2024
I sent this to the Queen of Hearts So the ECG is both STEMI negative and has no subtle diagnostic signs of occlusion. Non-STEMI guidelines call for “urgent/immediate invasive strategy is indicated in patients with NSTE-ACS who have refractory angina or hemodynamic or electrical instability,” regardless of ECG findings.[1]
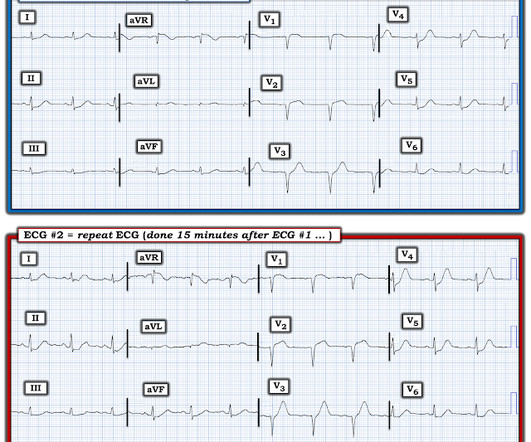
Dr. Smith's ECG Blog
MAY 31, 2023
Cath lab declined as it is not a STEMI." And now this finding is even formally endorsed as a "STEMI equivalent" in the 2022 ACC guidelines!!! Another myocardial wall is sacrificed at the altar of the STEMI/NonSTEMI mindset. Do NOT give it unless you are committed to the cath lab!! Cath attending is aware. It is a mass delusion.
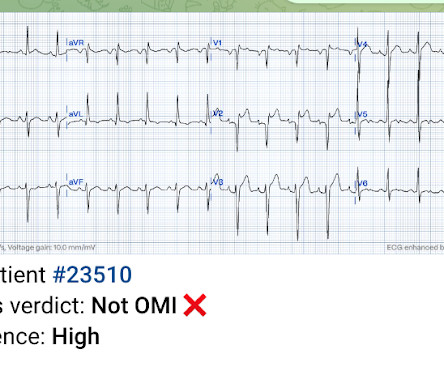
Dr. Smith's ECG Blog
OCTOBER 28, 2020
This ECG was texted to me with the implied question "Is this a STEMI?": I responded that it is unlikely to be a STEMI. Septal STEMI often has ST depression in V5, V6, reciprocal to V1. Then combine with clinical presentation and low pretest probability 2 Saddleback STEMIs A Very Subtle LAD Occlusion.T-wave wave in V1??
Dr. Smith's ECG Blog
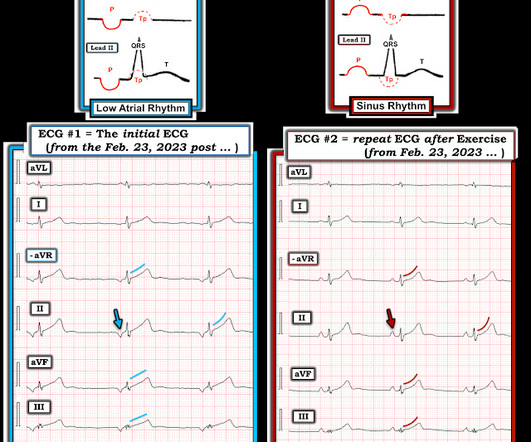
SEPTEMBER 29, 2023
In the available view of the sinus rhythm, we see normal variant STE which probably meets STEMI criteria in V4 and V5. In other words, the inferior "ST elevation" is due to the abnormal rhythm, and does not signify OMI or STEMI in any way. It is a known OMI mimic that we have shown on the blog many times.

Dr. Smith's ECG Blog
MAY 5, 2024
An undergraduate (not yet in medical school) who works as an ED technician (records all EKGs, helps with procedures, takes vital signs) and who reads this blog regularly arrived at work and happened to glance down and see this previously recorded ECG on a table in the ED. It was recorded at 0530: What do you think?
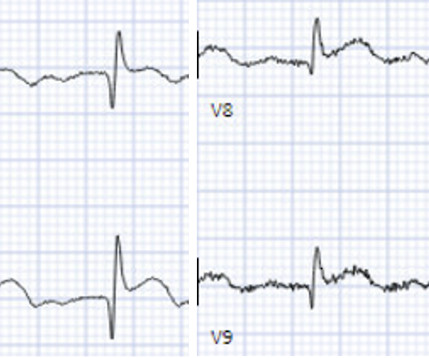
Dr. Smith's ECG Blog
MAY 27, 2024
The ECG did not meet STEMI criteria, and the final cardiology interpretation was “ST and T wave abnormality, consider anterior ischemia”. There’s only minimal ST elevation in III, which does not meet STEMI criteria of 1mm in two contiguous leads. But STEMI criteria is only 43% sensitive for OMI.[1]
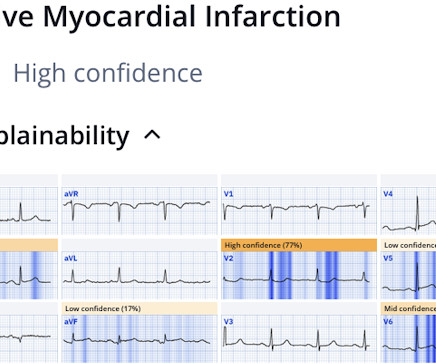
Dr. Smith's ECG Blog
MARCH 10, 2025
If we took this as the gold standard, we would conclude that the computer interpretation was safe and accurate at least accurate enough to not miss STEMI, and that physicians should not be interrupted to interpret it, because there would be no change in patient management. What is the gold standard for ECG interpretation: patient outcome!!!
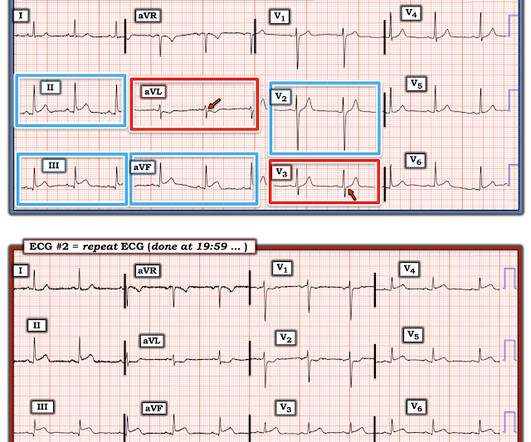
Dr. Smith's ECG Blog
JUNE 11, 2024
Now it is a full blown STEMI of 3 myocardial territories: inferior, posterior, and lateral But at least it does not call it "Normal." Learning Points: You cannot trust conventional algorithms even to find STEMI(+) OMI, even when they say "normal ECG." We have shown many examples of this on this blog.
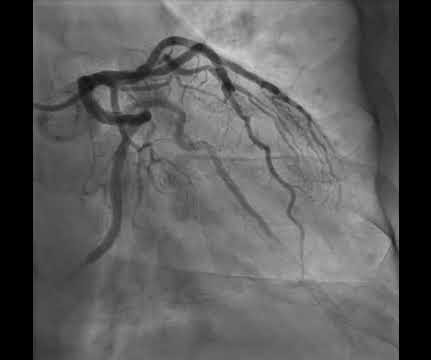
Dr. Smith's ECG Blog
AUGUST 2, 2024
This was a machine read STEMI positive OMI. Readers of this blog can easily appreciate the hyperacute T waves in the precordium, clearest in V1-V4. The meaning of this quote is that at times, something as obvious as the dramatic anterior lead ST elevation that we see in today's tracing is not the result of an acute LAD STEMI.
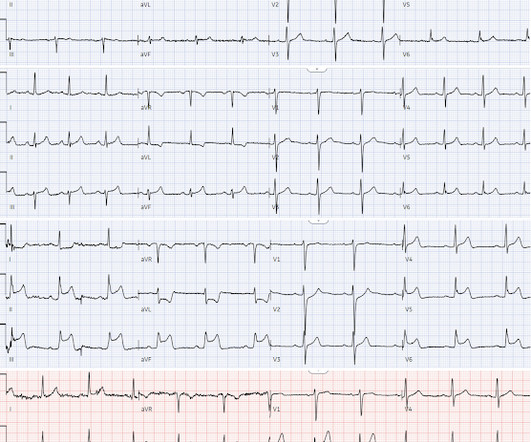
Dr. Smith's ECG Blog
JUNE 7, 2024
Obvious infero-postero-lateral STEMI(+)OMI, regardless of context Now let’s put them in order: what was the sequence? With serial ECGs that are ‘STEMI negative’ the physician could have waited for serial troponin levels or referred the patient as “non-STEMI”. What was the outcome and final diagnosis?

Dr. Smith's ECG Blog
JANUARY 20, 2024
This patient does not show up in the STEMI registry, and the time to reperfusion will likely not be identified as the problem that it was. The STEMI registry will show very high sensitivity of the ECG for STEMI, obscuring the fact the STEMI has low sensitivity for OMI Queen of Hearts sees it easily, like readers of the blog would.

Dr. Smith's ECG Blog
JULY 31, 2020
Meyers, Weingart and Smith published their OMI Manifesto — in which they extensively document the critically important concept that management of acute MI by separation into a “STEMI” vs “non-STEMI” classification is an irreversibly flawed approach.
Dr. Smith's ECG Blog
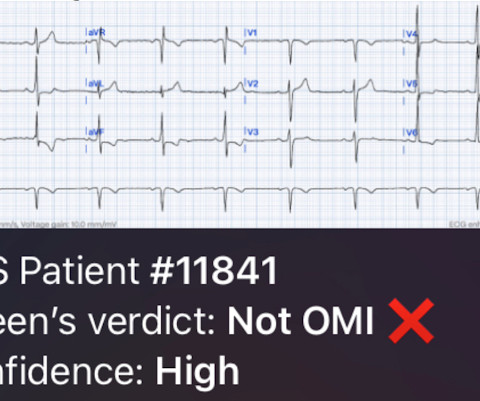
NOVEMBER 27, 2023
The biggest problem with STEMI criteria are false negatives – because this costs patient’s myocardium, with greater mortality and morbidity. For this reason, ECGs need first to be interpreted in isolation, and then applied to the patient. Could this false positive cath lab activation been prevented?
Expert insights. Personalized for you.
We have resent the email to
Are you sure you want to cancel your subscriptions?


Let's personalize your content